Osteoporosis Bones Health-2023
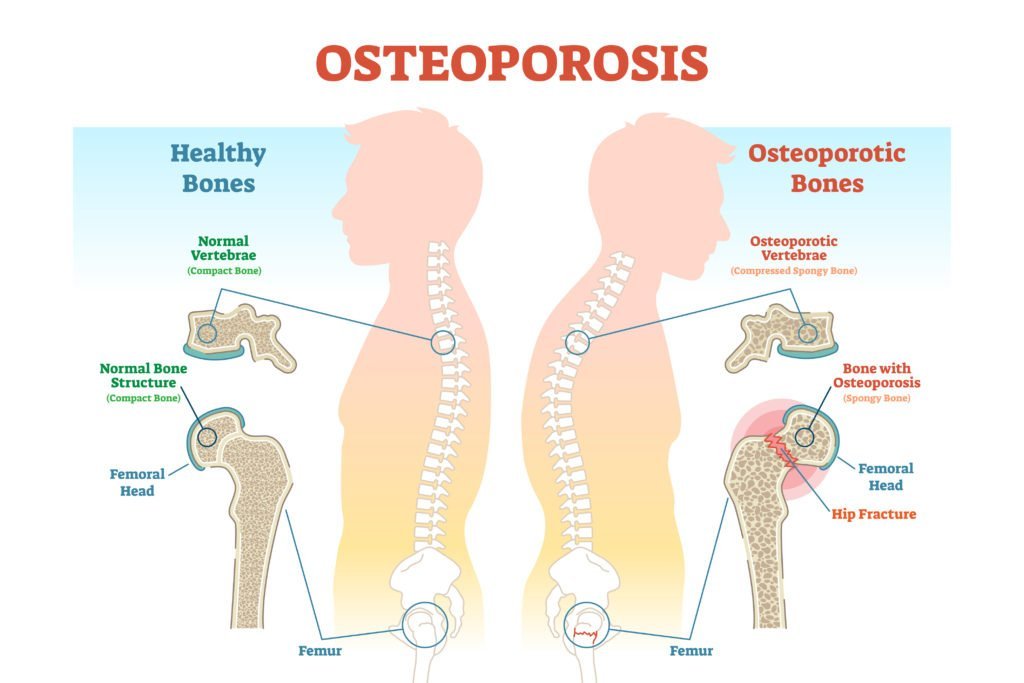
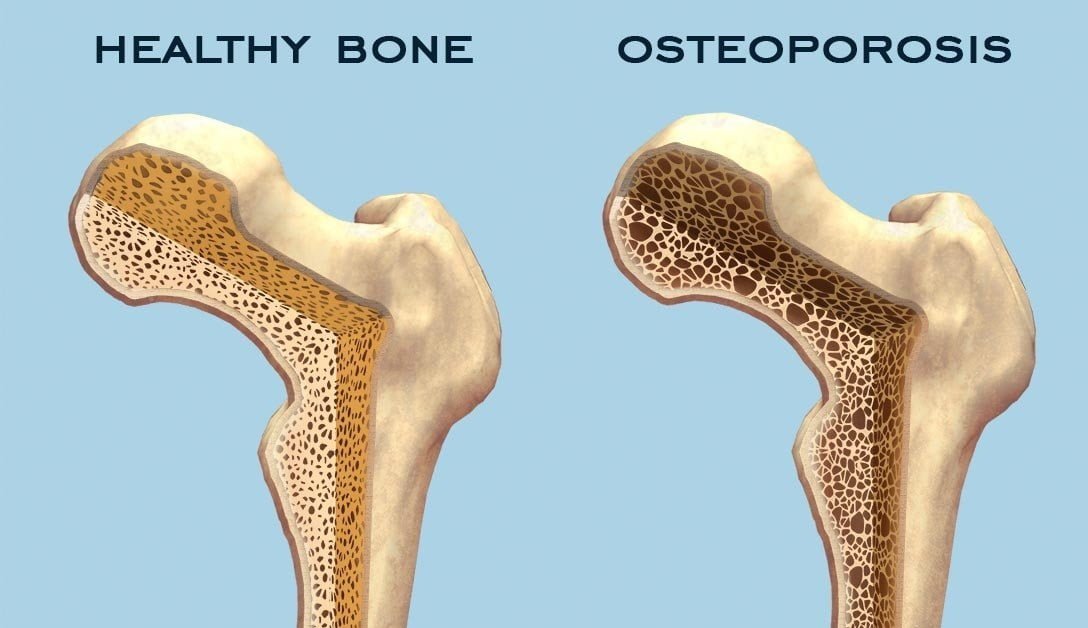
Osteoporosis Bones Health-2023 Osteoporosis Bones Health-2023. With osteoporosis, bones are brittle and often fracture or break. There are no symptoms before the osteoporosis bones shatter and the disease can only be detected through tests in your doctor’s office. You won’t automatically know your bones are getting thinner. White and Asian women past menopause are most susceptible to … Read more